Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (40): 6397-6402.doi: 10.3969/j.issn.2095-4344.2014.40.001
Tranexamic acid injection through articular cavity and discontinuous clip pipe after total hip arthroplasty: changes in bleeding amount
Fan Fu-cheng1, 2, Gui Bin-jie1
- 1Department of Orthopedics, First Affiliated Hospital, Anhui Medical University, Hefei 230001, Anhui Province, China; 2Department of Orthopedics, Hefei Municipal Second People’s Hospital, Hefei 230001, Anhui Province, China
-
Revised:2014-09-10Online:2014-09-24Published:2014-09-24 -
About author:Fan Fu-cheng, Physician, Department of Orthopedics, First Affiliated Hospital, Anhui Medical University, Hefei 230001, Anhui Province, China; Department of Orthopedics, Hefei Municipal Second People’s Hospital, Hefei 230001, Anhui Province, China
CLC Number:
Cite this article
Fan Fu-cheng, Gui Bin-jie. Tranexamic acid injection through articular cavity and discontinuous clip pipe after total hip arthroplasty: changes in bleeding amount[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(40): 6397-6402.
share this article
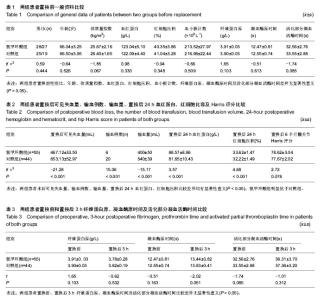
2.1 参与者数量分析 按意向性处理,纳入99例患者,分成两组,全部进入结果分析,无脱落。 2.2 基线资料比较 置换前氨甲环酸组和对照组患者性别比、年龄、体质量指数、血红蛋白、红细胞、血小板、纤维蛋白原、凝血酶原时间及活化部分凝血活酶时间比较差异均无显著性意义(P > 0.05),提示具有可比性,见表1。 2.3 失血量、输血例数、输血量、置换后24 h 血红蛋白、红细胞比容及Harris评分比较 表2提示使用氨甲环酸组出血量较未使用对照组平均少200 mL,输血病例较对照组明显减少,同时输血量也平均少150 mL左右,根据统计学原理,两组患者置换后失血量、输血例数、输血量、术后24 h血红蛋白、红细胞压积比较差异均有显著性意义(P < 0.05),氨甲环酸组明显优于对照组;而置换后6个月髋关节Harris评分及置换前、置换后3 h纤维蛋白原、凝血酶原时间及活化部分凝血活酶时间比较差异无显著性意义(P > 0.05),见表2,3。 置换后患者多次行彩超检查未见血栓形成,故证明关节腔注射氨甲环酸可有效减少出血及输血,并不增加置换后并发症。 2.4 置换后并发症发生情况 两组患者置换后14 d伤口均Ⅰ/甲级愈合,置换后多次(3,10,14 d)行下肢血管多普勒超声检查均未见出现明显下肢深静脉血栓形成,也未见其他严重内外科并发症发生。置换后6个月随访未发现下肢深静脉血栓或肺栓塞发生。"
| [1] Clavé A, Fazilleau F, Dumser D, et al. Efficacy of tranexamic acid on blood loss after primaryCementless total hip replacement with rivaroxaban thromboprophylaxis: A case-control Study in 70 patients. Orthop Traumatol Surg Res. 2012;98:484-490.
[2] Ronsencher N, Kerkkamp HE, Macheras G, et al. Orthopedic Surgery Transfusion hemoglobin European Overview(OSTHEO) study:blood management in elective knee and hip arth roplasty in Europe. Transfusion. 2003;43: 459-469.
[3] Lee YC, Park SJ, Kim JS, et al. Effect of tranexamic acid on reducing postoperative blood loss in combined hypotensive epidural anesthesia and general anesthesia for total hip replacement. J Clin Anesth. 2013;25:393-398.
[4] Borghi B, Borghi R. Blood-saving techniques. Transplant Proc. 2011;43:333-337.
[5] Huang F, Wu D, Ma G, et al. The use of tranexamic acid to reduce blood loss and transfusion in major orthopedic surgery: a meta-analysis. J Surg Res. 2014;186(1):318-327.
[6] Bierbaum BE, Callaghan JJ, Galante JO, et al. An analysis of blood management in patients having a total hip or knee arthroplasty. J Bone Joint Surg Am.1999;81(1):2.
[7] Wei W, Wei B. Comparison of Topical and Intravenous Tranexamic Acid on Blood Loss and Transfusion Rates in Total Hip Arthroplasty. J Arthroplasty. 2014.
[8] Engoren M, Mitchell E, Perring P, et al. The effect of erythrocyte blood transfusions on survival after surgery for hip fracture. J Trauma. 2008;65(6):1411-1415.
[9] Bochicchio GV, Napolitano L, Joshi M, et al. Outcome analysis of blood product transfusion in trauma patients: a prospective, risk-adjusted study. World J Surg. 2008;32(10): 2185-2189.
[10] Weber EW, Slappendel R, Prins MH, et al. Perioperative blood transfusion and delayed wound healing after hip replacement surgery: effects on duration of hospitalization. Anesth Analg.2005;100(5):1416-1421.
[11] Hawi N, Kendoff DO, Hessling U, et al. Effectiveness of an autologous transfusion system following cemented and non-cemented revisions of total hip arthroplasty. Int Orthop. 2014;38(8):1603.
[12] Horstmann WG, Swierstra MJ, Ohanis D, et al. Favourable results of a new intraoperative and postoperative filtered autologous blood re-transfusion system in total hip arthroplasty: a randomised controlled trial. Int Orthop. 2014;38(1):13.
[13] Shander A, Hofmann A, Ozawa S, et al. Activity-based costs of blood transfusions in surgical patients at four hospitals. Transfusion. 2010;50(4):753.
[14] Alshryda S, Mason J, Sarda P, et al. Topical (Intra-Articular) Tranexamic Acid Reduces Blood Loss and Transfusion Rates Following Total Hip Replacement A Randomized Controlled Trial (TRANX-H). J Bone Joint Surg Am. 2013;95:1969.
[15] Wind TC, Barfield WR, Moskal JT. The Effect of Tranexamic Acid on Transfusion Rate in Primary Total Hip Arthroplasty. J Arthroplasty. 2014;29(2):387-389.
[16] Martin JG, Cassatt KB, Kincaid-Cinnamon KA, et al. Topical Administration of Tranexamic Acid in Primary Total Hip and Total Knee Arthroplasty. J Arthroplasty. 2013.
[17] Konig G, Hamlin BR, Waters JH. Topical Tranexamic Acid Reduces Blood Loss and Transfusion Rates in Total Hip and Total Knee Arthroplasty. J Arthroplasty. 2013;28:1473.
[18] Fiechtner BK,Nuttall GA,Johnson ME,et al.Plasma tranexamic acid concentrations during cardiopulmonary bypassv.Anesth Analg. 2001;92(5):1131-1136.
[19] Hynes MC,Calder P,Rosenfeld P,et al. The use of tranexamic acid to reduce blood loss during total hip arthroplasty:an observational study. Ann R Coil Surg Engl. 2005;87(2): 99-101.
[20] Fiechtner BK,Nuttall GA,Johnson ME,et al.Plasma tranexamic acid concentrations during cardiopulmonary bypassv.Anesth Analg. 2001;92(5):1131-1136.
[21] Singh J, Ballal MS, Mitchell P, et al.Effects of tranexamie acid on bloodloss during THA. J Orthop Surg. 2010;18(3):282-286.
[22] Henry DA, Carless PA, Moxey AJ, et al. Anti-fibrinolytic use for Minimising perioperative allogeneic blood transfusion. Cochrane Database Syst Rev. 2011;3:CD001886.
[23] Royston D. Blood-sparing drugs:aprotinin,tranexamic acid,andepsilon-aminocaproic acid. Int Anesthesiol Clin. 1995;33(1):155-179.
[24] Alshryda S,Sarda P,Sukeik M,et al.Tranexamic acid in total knee replacement:a systematic review and meta-analysis. J Bone Joint Surg Br. 2011;93(12):1577-1585.
[25] Leveille GA, Pardini RS, Tillotson JA. Influence of medium-chain triglycerides on lipid metabolism in the chick. Lipids. 1967;2(6): 461-466.
[26] Hynes MC, Calder P, Rosenfeld P, et al.The use oftYaneKamlc acid to reduce blood 10ss during total hip arthmplasty!an observational study. Ann R Coll Surg Engl. 2005;87(2):99-101.
[27] Benoni G, Fredin H, Knebel R, et al. Blood conservation with tranexamic acid in total hip arthroplasty: a randomized, double-blind study in 40 primary operations. Acta Orthop Scand. 2001;72:442.
[28] Husted H, Blønd L, Sonne-Holm S, et al. Tranexamic acid reduces blood loss and blood transfusions in primary total hip arthroplasty: a prospective randomized double-blind study in 40 patients. Acta Orthop Scand. 2003;74:665.
[29] Lemay E, Guay J, Côté C, et al. Tranexamic acid reduces the need for allogenic red blood cell transfusions in patients undergoing total hip replacement. Can J Anaesth. 2004;51: 31.
[30] Johansson T, Pettersson LG, Lisander B. Tranexamic acid in total hip arthroplasty saves blood and money: a randomized, double-blind study in 100 patients. Acta Orthop. 2005;76:314.
[31] Ido K, Neo M, Asada Y, et al. Reduction of blood loss using tranexamic acid in total knee and hip arthroplasties. Arch Orthop Trauma Surg. 2000;120:518.
[32] Molloy DO,Archbold HA,Ogonda L,et al.Comparison of topical Fibrin spray and tranexamic acid on blood loss after total knee replacement:a prospective,randomised controlled trial.J Bone Joint Surg Br. 2007;89(3):306-309.
[33] Hynes M,Calder P,Scott G. The use of tranexamic acid to reduce blood loss during total knee arthroplasty. Knee. 2003; 10(4):375-377.
[34] Wind TC, Barfield WR, Moskal JT. The effect of tranexamic acid on transfusion rate in primary total hip arthroplasty. J Arthroplasty. 2014;29(2):387.
[35] Kim YH, Cho SH, Kim RS. Drainage versus nondrainage in simultaneous bilateral total hip arthroplasties. J Anhroplaty. 1998;13(2):156-161.
[36] Southern EP,Huo MH,Mehta JR,et al. Unwashed wound drainage blood. What are wegiving ourpatients. Clin Orthop. 1995;320:235-246.
[37] Lozano M,Basora M,Peidro L,et al.Effectiveness and safety of tranexamic acid administration during total knee arthroplasty. Vox Sang. 2008;95(1):39-44.
[38] Lerler BK.Ultrasonngraphy and diagnosis of venous thromboem bolism. Circulation. 2004;109(12 Supp1):19-24.
[39] Barnes CL, Nelson CL, Nix ML, et al. Duplex scanning versus venography as a screening examination in total hip arthroplasty patients. Clin Orthop Relat Res. 1991;(271):180.
[40] Grady-Benson JC, Oishi CS, Hanson PB, et al. Routine postoperative duplex ultrosonography screening and monitoring for the detection of deep vein thrombosis. Clin Orthop Relat Res. 1994;307:130.
[41] Tremaine DM, Choroszy CJ, Menking SA. Deep vein thrombosis in the total hip arthroplasty patient after hospital discharge. J Vase Tech. 1992;16:23.
[42] Sukeik M, Alshryda S,Haddad FS,et al. Systematic review and meta-analysis of the use of tranexamic acid in total hip replacement. J Bone Joint Surg Br. 2011;93(1):39-46. |
| [1] | Yuan Wei, Zhao Hui, Ding Zhe-ru, Wu Yu-li, Wu Hai-shan, Qian Qi-rong. Association between psychological resilience and acute mental disorders after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1015-1019. |
| [2] | Ye Xiang-yang, Sun Xiang, Tang Li-xin, Zhen Ping, Geng Bin, Wang Hua-lei, Zhao Yu-guo. Acetabular liner wear of cross-linked versus conventional polyethylene for total hip arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1143-1148. |
| [3] | Liang Xin, Wang Heng, Li Xian-rong. Preoperative application of alprazolam for patients with anxiety and depression and pain after total knee arthroplasty: its safety and effectiveness [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 985-992. |
| [4] | Shi Bin, An Jing, Chen Long-gang, Zhang Nan, Tian Ye . Influencing factors for pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 993-997. |
| [5] | Wang Xian-xun. Impact of local compression cryotherapy combined with continuous passive motion on the early functional recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 998-1003. |
| [6] | Lu Yao-jia, Xiong Chuan-zhi, Li Xiao-lei, Hu Han-sheng, Chen Gang, Wang Qiang, Lu Zhi-hua. Comparison of two methods for reducing blood loss during total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1004-1008. |
| [7] | Tian Hai-tao, Wang Yuan-he, Tian Shao-qi, Zhang Xu-teng, Sun Kang. Effects and safety assessment of methylprednisolone on postoperative nausea and vomiting and pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 335-339. |
| [8] | Jia Jin-ling, Dong Yu-zhen. Finite element analysis of prosthesis position during hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 401-405. |
| [9] | Lu Zhong-lin, Cao Zhi-qiang, Gao Guo-liang, Jing Qing-ling, Zhang Wei, Huang Yong. Incidence and risk factors of deep vein thrombosis during waiting period before operation for calcaneal fractures by ultrasound elastography [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 423-427. |
| [10] | Zhu Shi-bai, Zhai Jie, Jiang Chao, Ye Can-hua, Chen Xi, Weng Xi-sheng, Qian Wen-wei. Application of “enhanced recovery after surgery” in the perioperative period of total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 456-463. |
| [11] | Wei Zhi-hui, Zhang Zhong-zu, Zhang Ming-hua. Intravenous combined with topical application of tranexamic acid in primary total hip arthroplasty: a meta-analysis of efficacy and safety [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 464-470. |
| [12] | Hu Jun, Zhang De-qiang, Tang Xin. Postoperative quality of life of internal fixation versus hemiarthroplasty for femoral neck fractures in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 2953-2960. |
| [13] | Sun Hao, Wei Jun-qiang, Liu Li-rui, Yan Shi, Jin Yu, Feng Zhen. Time of lower extremity deep venous thrombosis after hip arthroplasty in senile patients with osteoporotic femoral neck fractures [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 2961-2965. |
| [14] |
Gao Wei-lu, Li Hong, Liu Bi-quan, Hu Yong, Liu Jing-jun, Yin Li, Liu Hu, Mei Bin, Yin Zong-sheng.
Analgesic effect of femoral and sciatic nerve block under multimodal analgesia in total knee arthroplasty
|
| [15] | Bai Zhao-hui, Zhang Ying, Yin Qing-shui, Xia Hong, Wang Jian-hua, Xu Jun-jie. Navigational template applied in the orthopaedic field in China: a bibliometric analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 3023-3030. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||